The regional office for Europe of the World Health Organization (WHO) defined health literacy as a connection with literacy that involves an individual’s knowledge, motivation and competencies to access, understand, appraise, and apply health information to make informed judgments and decisions about healthcare, disease prevention and health promotion in their daily lives to maintain or improve quality of life during the life course1. As academic interest in health literacy continues to grow, an increasing body of research highlights its role as a foundational element in shaping health promotion policies and programs. Health literacy measurement tools are essential for assessing health status, guiding behavior change, promoting self-reflection, and comparing group-level differences—key components for effective individual health management2.
Currently, scholars have used health literacy to construct theoretical models that clarify the intricate association between health literacy and health outcomes and identify the factors that affect health literacy. The literature proposes several theoretical models. For example, one of the most commonly cited models is the “Newest Vital Sign” model, which focuses on how health literacy is related to health outcomes3. The “Interactive Health Literacy” model highlights the interaction between individuals and their environment and suggests that health literacy is not solely an individual’s characteristic but is also influenced by external factors such as the availability of health information and resources4. Moreover, the “Health Literacy and Self-Management” model emphasizes the function of health literacy in self-management behaviors such as medication adherence and healthy lifestyle choices, suggesting that individuals with higher health literacy are more inclined to interact with such behaviors5. However, to apply these theories in practice, it is essential to measure health literacy accurately.
Through a literature search, we have identified 47 health literacy assessment tools, which can be categorized into four types: comprehensive assessment tools, skills assessment tools, disease-specific assessment tools, and population-specific assessment tools6. Comprehensive assessment tools, such as the European Health Literacy Survey Questionnaire1, evaluate multiple aspects of an individual’s health literacy. Skills assessment tools, such as the Test of Functional Health Literacy in Adults7 and Health Literacy Skills Instrument8, evaluate an individual’s ability to perform specific health-related skills. Disease-specific assessment tools, such as the Diabetes Health Literacy Scale9, assess an individual’s capability to comprehend and manage health-related information about a particular disease or condition. Population-specific assessment tools, such as the Childhood Health Literacy Scale, are designed to evaluate the health literacy of specific populations10.
The most widely used questionnaire for long-term monitoring and comparing health literacy among the general and specific populations is the European Health Literacy Survey Questionnaire (HLS19-Q47) proposed by the International Coordination Center (ICC) of WHO Action Network on Measuring Population and Organizational Health Literacy (M-POHL)11. At present, this scale has been widely used in Europe, Asia, and South America as a metric of health literacy and to facilitate cross-country comparisons1,12,13. The HLS19-Q47 is a self-report tool that assesses perceived difficulty in 47 tasks related to health care, disease prevention, and health promotion at four stages (access, understand, appraise, and apply) of information processing. The tool employs a scale ranging from “very easy” to “very difficult” to evaluate both individual skills and the fit between personal competencies and the complexity of the situation1.
Since the release of the HLS19-Q47, scholars worldwide have utilized it as a standard tool for measuring health literacy and conducting research across diverse populations. A European study utilizing the HLS19-Q47 revealed substantial differences in health literacy levels among countries. At least 12% of the participants had deficient health literacy, and nearly 50% had limited health literacy, with a large variation in levels among countries (29–62%)1. The survey data showed a socioeconomic gradient in health literacy, with those of lower social status, education, economic deprivation, and younger ages having more individuals with low health literacy. The study also used the Newest Vital Sign (NVS)-Test, a validated objective measure of health literacy3, for comparison and validation, and found similar results to the general index of HLS19-Q47. Previous studies using HLS19-Q47 have indicated that low health literacy is linked to adverse health status1,14, increased healthcare service utilization, longer hospital stays1,15, and higher mortality rates15,16. Moreover, low health literacy has been linked to unhealthy behaviors such as smoking, inadequate physical activity, and reduced use of preventive care services17,18,19. Thus, HLS19-Q47 is a mature and widely used tool for measuring health literacy among populations internationally.
While health literacy is crucial for personal and societal health, its development is slow in China, especially in the measurement tools. In the past, Chinese scholars have extensively researched health literacy using the Chinese Citizens Health Literacy Questionnaire (CCHLQ) for residents, devised by the Chinese Health Education Center20. However, this questionnaire has limitations as it comprises 80 items and is limited to individuals under the age of 69, restricting its application and expansion to 21. Meanwhile, due to language barriers, the CCHLQ is only used in China and has not been promoted to other countries, making it difficult to compare and research health literacy levels among nations. Therefore, it is crucial to use a comparable health literacy scale to measure the level of health literacy in China and construct a health literacy empirical model.
At present, no scholars in mainland China have used HLS19-Q47 to study health literacy. Although the HLS19-Q47 has been applied in Taiwan12, slight differences in the language environment and cultural context between Taiwan and mainland China make the Taiwanese version of the HLS19-Q47 not applicable in China. Therefore, before conducting this study, our team invited five translation experts to translate the HLS19-Q47 into Chinese, followed by back-translating it for accuracy. We also adapted the questionnaire culturally through a small-scale survey. The Chinese version of the HLS19-Q47 passed the accuracy and clarity assessment by 21 experts and professors in different fields. Finally, we conducted a large-scale survey in China to evaluate the reliability and validity of the HLS19-Q47, concluding that it can serve as an important tool for assessing the health literacy of Chinese residents and enabling comparisons with other countries21.
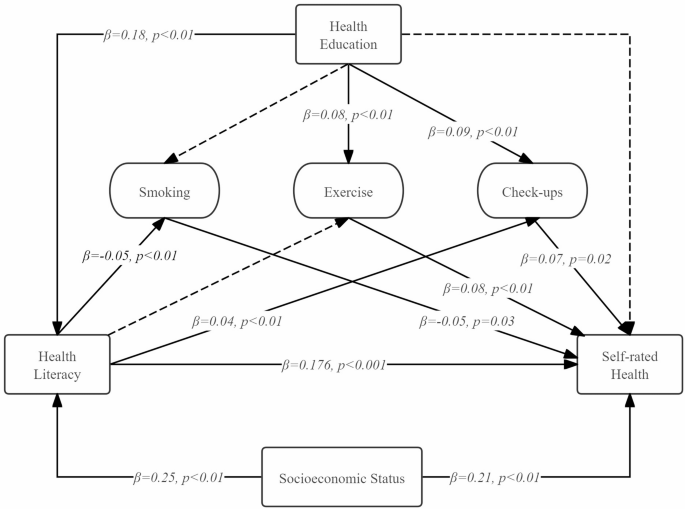
Previous studies by Chinese researchers often develop empirical models based on an established conceptual framework. However, these models are limited by issues in variable specification and theoretical refinement. To address these limitations, the present study proposes the Health Literacy Empowerment Model (HLEM), which integrates key determinants of health literacy, including health education, health behaviors, self-rated health, and socioeconomic status, into a comprehensive framework that spans health outcomes, self-management, and health promotion. Building upon existing theoretical and statistical evidence, this study adapts the HLEM to an individual level in the context of Guangzhou, China, using HLS19-Q47 as the primary assessment tool. In this model, health literacy is defined as an individual’s ability, with socioeconomic status and health education serving as external determinants. Self-rated health is used as an indicator of health outcomes, and health behaviors reflect self-management practices. This refined approach enhances both theoretical clarity and empirical relevance in health literacy research.
Given the complexity of the relationships among multiple latent variables and observed variables in HLEM, the traditional regression model itself is insufficient to capture the entire range of the dynamics among the variables. Therefore, in this study, in addition to using the regression model to analyze the correlation between variables, the Structural Equation Model (SEM) is also adopted to evaluate the measurement properties of the configuration and investigate the structural relationship between the variables at the same time. This method is conducive to a more comprehensive understanding of the interactions among different factors within the proposed framework.
The arrangement of this article is as follows. We first explored the association between demographic factors and health literacy. We then examined the connections between health education and socioeconomic status with health literacy and self-rated health status. We also analyzed the associations between health literacy and health education and health behaviors (including alcohol consumption, smoking, physical activity, and health check-ups), as well as the relationships between these behaviors and self-rated health status. Finally, we utilized SEM to construct HLEM.
link